Quick answer: Frozen shoulder is up to several times more common in women aged 40 to 60 than in men of the same age. The likely reason: declining estrogen affects the collagen and connective tissue that lines the shoulder capsule. A 2023 Duke single-center analysis of 1,952 menopausal women found women on hormone replacement therapy had a 3.95% rate of adhesive capsulitis vs 7.65% for women not on HRT — roughly half the incidence. The frozen shoulder menopause connection is real, under-discussed, and treatable.
The 60-second version
If your shoulder froze around the same time your periods got weird
If your shoulder started locking up around the same time your periods got irregular, your sleep got worse, and your hips ache when you stand up from the couch — that is not a coincidence. That is a constellation. The frozen shoulder menopause pattern is one of the most consistent presentations in midlife musculoskeletal medicine, and it is also one of the most consistently missed.
You are not imagining it. You did not sleep on it wrong. The shoulder hurts at night, deep in the joint, in a way ibuprofen barely touches. You can't put your bra on without an awkward over-the-head workaround. Range of motion shrinks week by week, and the doctor's office sends you home with a steroid injection and a PT referral without ever asking when your last period was. This pattern has a name in the literature — perimenopause frozen shoulder — and it is increasingly recognized as a distinct presentation rather than a coincidence.
This article is the conversation you should have been offered: the mechanism, the study most general menopause blogs don't cite, the staging, the treatment menu in honest order, and what the frozen shoulder menopause connection means for whether HRT belongs on your list.
"Wait, isn't frozen shoulder just an injury thing?"
This is the pattern interrupt. Most women hear "frozen shoulder" and assume they slept on it wrong, lifted something heavy, or have a rotator cuff thing. The textbook reality, per the American Academy of Family Physicians 2019 review on adhesive capsulitis: the majority of frozen shoulder cases — especially in women aged 40 to 60 — have no trauma history at all. The shoulder just slowly, mysteriously, freezes.
This is the diagnostic clue most clinicians don't say out loud: when a woman in her late 40s arrives at the orthopaedist with a stiff, painful shoulder and no story, the differential is dominated by adhesive capsulitis driven by something systemic. Diabetes, thyroid disease, and — increasingly recognized — perimenopausal estrogen loss are the usual suspects. A shoulder that froze without an injury is a shoulder telling you something about the rest of the body. Frozen shoulder perimenopause cases follow this pattern almost universally: no injury, no overuse, no clear story, just a slow capsular shutdown that maps onto the hormonal transition.
That reframe matters because it changes the question from "what did I do to my shoulder?" to "what is happening to my connective tissue?" — and that second question is where the menopause hormone story enters.

The mechanism: how estrogen affects the shoulder capsule
The shoulder is held together by the glenohumeral joint capsule — a sleeve of connective tissue rich in collagen and lined with fibroblasts (the cells that make collagen). When the hormonal environment is healthy, the capsule stays loose, flexible, and inflammation-free; it stretches when you reach overhead and rebounds when you drop your arm.
Estradiol — the dominant estrogen during reproductive years — has well-documented effects on this connective tissue:
- Collagen synthesis. Estrogen receptors are expressed on fibroblasts throughout the joint capsule, tendons, and ligaments. Estradiol upregulates type I and type III collagen production and supports orderly cross-linking.
- Anti-inflammatory effect. Estradiol shifts the immune environment toward less inflammation. Estrone — the dominant estrogen after menopause — is comparatively pro-inflammatory.
- Endothelial function. Estrogen supports the small blood vessels feeding connective tissue, keeping fibroblasts well-perfused and quiescent rather than activated.
- Pain modulation. Estrogen receptors on peripheral nerves and in the central nervous system modulate pain processing; estrogen withdrawal can amplify musculoskeletal pain.
When estrogen drops through perimenopause and falls off a cliff at menopause, every one of those protective effects weakens at once. The 2025 Journal of Clinical Medicine review on frozen shoulder as a systemic disorder sums up the cascade: "estrogen decline may shift the immune environment toward a pro-inflammatory and profibrotic state, favoring the activation of fibroblasts and excessive collagen production in the shoulder capsule."
That last phrase — excessive collagen production in the shoulder capsule — is the pathology of frozen shoulder. The capsule thickens, contracts, scars. Range of motion shrinks. Pain peaks at night when the inflamed capsule has nowhere to expand into. None of it makes sense as a local injury; all of it makes sense as a systemic story playing out in one joint.
This is why the frozen shoulder menopause link shows up so consistently in the same age window — and why physical therapy alone, while it helps, often feels like rowing upstream against a hormonal current.
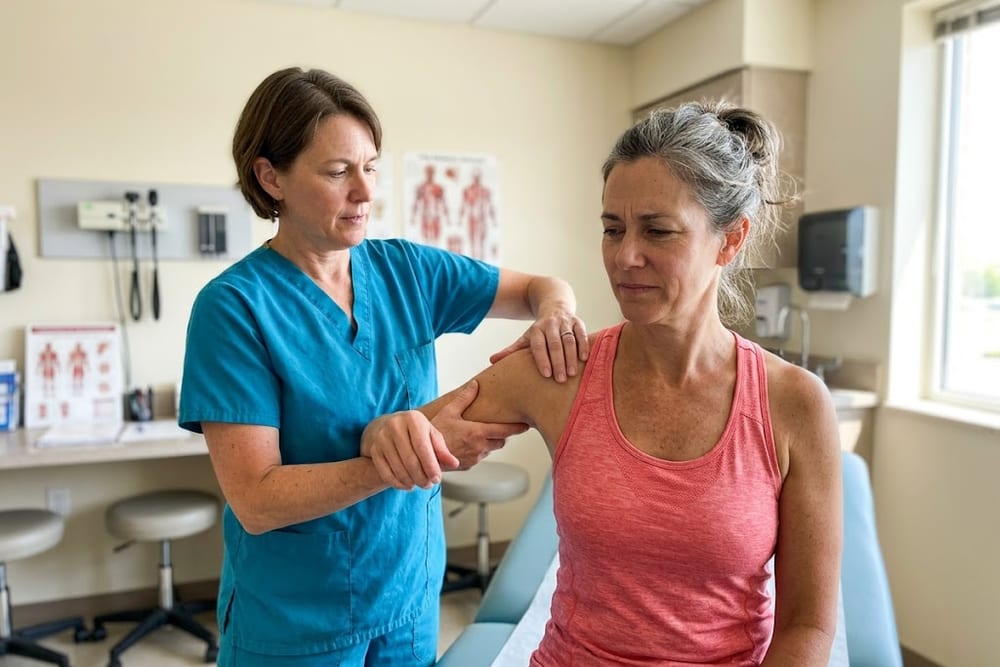
Why doctors don't tell you this: the 2023 Duke HRT analysis
In 2022 a Duke team led by Dr. Jocelyn Wittstein (orthopaedic surgery) and Dr. Anne Ford (obstetrics & gynecology) presented data at the North American Menopause Society annual meeting. Published in 2023 as: Saltzman E, Kennedy J, Ford A, Wittstein JR, et al. "Is Hormone Replacing Therapy Associated with Reduced Risk of Adhesive Capsulitis in Menopausal Women?" Orthop J Sports Med. 2023;11(7 suppl 3):2325967123S00174.
Women not on HRT had 99% greater odds of adhesive capsulitis than women on HRT (OR 1.99; 95% CI 0.86–4.58; p = 0.11). The result fell short of statistical significance because of sample size, but the effect direction was clean and the absolute incidence nearly halved. Dr. Wittstein, summarizing the rationale to Duke Health: "estrogen plays a role in stimulating bone growth, reducing inflammation, and promoting connective tissue integrity."
Why don't doctors tell you about this? The menopause-shoulder bridge crosses two specialties — orthopaedics and gynecology — and lives in neither textbook. The frozen shoulder menopause connection is rigorously plausible, observationally supported, and clinically under-communicated. That is the gap this article closes.

The three stages of frozen shoulder
Frozen shoulder unfolds in three classical phases. The total course untreated is roughly one to three years, though more recent reviews (Ochsner Journal 2024; Clinical Guidelines in the Management of Frozen Shoulder) caution that complete spontaneous recovery is less common than the older textbooks suggested.
| Stage | Duration | What it feels like |
|---|---|---|
| 1. Freezing | 2–9 months | Progressive pain, especially at night. Sleep is the first casualty. Range of motion shrinks. Reaching overhead, behind your back, or across your body becomes painful before it becomes impossible. |
| 2. Frozen | 4–12 months | Pain levels off, but stiffness peaks. The shoulder feels locked. External rotation is the worst-affected motion. Daily tasks — bra, hair, seatbelt — get redesigned around what the shoulder will allow. |
| 3. Thawing | 6–24 months | Range of motion gradually returns. Pain fades. Most women regain most function, though residual stiffness on extreme external rotation can linger for years. |
The honest framing: the freezing stage is the worst, and that is when most women come in. The temptation in clinic is to confirm the diagnosis, prescribe physical therapy, hand out a steroid injection, and send you on your way. That is a reasonable plan for the shoulder. It is an incomplete plan for the woman whose connective tissue is also affecting her hips, fingers, and night sleep — which brings us to the broader perimenopause joint pain picture and the full frozen shoulder menopause clinical context.
Why women in midlife are uniquely affected
Adhesive capsulitis affects 2 to 5% of the general population over a lifetime, per the AAFP. That number understates the female midlife reality: "most patients diagnosed with adhesive capsulitis are women between 40 and 60 years of age." The lifetime risk for a woman entering perimenopause is materially higher than the headline number suggests.
Why this group, why this window? The answer is hormonal but multifactorial:
- Estrogen withdrawal. The mechanism above. The single most common reason a 50-year-old woman with no shoulder injury develops a frozen shoulder.
- Type 2 diabetes. A strong, independent risk factor — diabetic women have roughly 5x the adhesive capsulitis risk of non-diabetic women.
- Thyroid disease. Subclinical hypothyroidism is more common after menopause and independently associated with frozen shoulder.
- Dupuytren's contracture. A fibrotic disorder of the hand that travels in the same fibrosing-tissue family.
- Immobilization. Estrogen-poor connective tissue does not tolerate immobilization well; even a brief sling for a wrist sprain can seed a frozen shoulder.
The same hormonal shift that drives the frozen shoulder menopause pattern also drives menopause weight gain, perimenopause hip pain when you stand up from a chair, perimenopause joint pain in the hands and feet, and the broader pattern doctors loosely call "menopause and joint pain." Menopause and joint pain typically arrives as a constellation. New ache in your hips, stiffness in your fingers in the morning, and a frozen shoulder all at once — that is one disease with one driver, not three coincidences.
Perimenopause hip pain shares the same fibroblast-driven mechanism that produces perimenopause frozen shoulder, expressed in a different joint. Perimenopause joint pain in the small joints is the diffuse version of the same connective-tissue story. Frozen shoulder perimenopause is the loudest form. Treating one without considering the others tends to leave women cycling through specialists.
What actually treats frozen shoulder — in honest order
Here is the evidence-ranked treatment menu, with the part most general menopause blogs leave off (HRT) included rather than skipped.
1. Physical therapy — the gold standard, slow but reliable
Daily stretching, range-of-motion work, and supervised PT remains the foundation for any perimenopause frozen shoulder presentation. The 2024 Ochsner Journal review concluded that PT improves shoulder pain, range of motion, and function, with the strongest effect when combined with a corticosteroid injection in the freezing phase. The downside: PT is slow. Expect 6 to 12 months for meaningful gains, longer if started during the painful freezing stage. Women whose menopause and joint pain extend beyond the shoulder often benefit from a generalised mobility program rather than shoulder-only PT.
2. Intra-articular corticosteroid injection — short-term relief
An ultrasound-guided steroid injection into the joint reduces pain quickly and creates a window in which PT actually works. Best used early — during the freezing phase — when inflammation is the dominant problem. Effect tapers around 12 weeks; some women need a second injection.
3. Hydrodilatation — under-prescribed, increasingly evidence-supported
A less commonly known procedure: the joint capsule is distended with sterile saline (often with a steroid and local anesthetic) until the capsule literally stretches. Recent 2024-2026 trials (including a large-volume protocol under suprascapular nerve block) show meaningful range-of-motion gains at six months and beyond. Worth asking your orthopaedist about specifically — many women with perimenopause frozen shoulder aren't offered it.
4. Manipulation under anesthesia & arthroscopic capsular release — last resort
Under general anesthesia, the surgeon firmly mobilizes the shoulder through full range of motion or arthroscopically releases the contracted capsule. Reserved for cases that have failed PT and injection at the 12-to-18-month mark. Effective but carries a small risk of fracture or rotator cuff injury. Surgical release addresses the local fibrosis but does nothing for the systemic environment that produced the frozen shoulder menopause picture — which is why surgical outcomes still leave the contralateral shoulder vulnerable.
5. Hormone replacement therapy — the differentiated angle
This is the option most orthopaedic visits skip, even though the 2023 Duke data put it on the table. HRT — typically transdermal estradiol plus oral micronized progesterone for women with a uterus — addresses the underlying systemic environment driving the capsular fibrosis. The Duke analysis suggests HRT may roughly halve the incidence of new adhesive capsulitis. It will not melt an existing frozen shoulder overnight, but for a woman with overlapping menopause symptoms the evidence supports a serious conversation — particularly about protecting the contralateral shoulder.
For the cost picture, our HRT cost comparison walks through the brand vs compounded math. ClearedRx prescribes estradiol patches, estradiol tablets, oral progesterone, and estradiol vaginal cream.
"Estrogen plays a role in stimulating bone growth, reducing inflammation, and promoting connective tissue integrity." — Dr. Jocelyn Wittstein, Duke Department of Orthopaedic Surgery (2023 NAMS / Duke Health press release)
What women are actually saying about it
If you read the major midlife support communities — the menopause subreddit, perimenopause-focused Facebook groups, NAMS patient-facing forums — the same paragraph appears over and over, with different names attached. Many women in midlife support communities describe the same arc, almost word-for-word, when they realize their menopause and joint pain and their frozen shoulder are part of the same story:
"I thought I'd injured myself but my doctor couldn't find anything. It just hurt. PT helped a little. The MRI was clean. What no one ever mentioned was the perimenopause connection — and now that I'm reading about it, half the women I know my age have had this and nobody told them either."
The frozen shoulder menopause pattern is statistically dominant in women 40 to 60, but clinically under-discussed, so it lives in peer support before it lives in clinic notes. The Duke study matters because it pulls the pattern out of the whisper network and into a journal an orthopaedist can cite.

If your shoulder froze around perimenopause: how to think about HRT
Frozen shoulder by itself is not a stand-alone reason to start HRT — it is a meaningful data point. If your shoulder froze around the same time other perimenopause symptoms started (irregular periods, hot flashes, night sweats, sleep that won't hold, finger and hip stiffness, mood changes, vaginal dryness), those symptoms together typically justify HRT, not the shoulder alone.
The frozen shoulder menopause overlap is a useful prompt to step back and look at the whole picture. Many patients arrive after a year of "shoulder problem, sleep problem, mood problem, hip problem" — four visits to four clinicians — and discover those are not four problems. They are one problem with four expressions, and one prescription regimen often addresses all of them at once.
ClearedRx prescribes bioidentical estradiol (patch, gel, oral, or vaginal) plus oral micronized progesterone where appropriate, starting at $19 per month. Online intake, 24-hour MD review, ships nationwide. The qualification check is free and takes about 3 minutes.
Frequently asked questions
Can frozen shoulder be caused by perimenopause?
Yes — and the timing is one of the strongest clues. Frozen shoulder peaks in women between the ages of 40 and 60, the same window as perimenopause and early postmenopause. Estrogen helps maintain the collagen and connective tissue that lines the shoulder capsule, so when estrogen drops the capsule becomes more vulnerable to inflammation and fibrosis. Most cases of perimenopause frozen shoulder have no trauma history; the hormone shift is the suspected driver. Frozen shoulder perimenopause cases also tend to cluster with other perimenopause joint pain complaints — fingers, hips, knees — confirming the systemic connective-tissue story.
Does HRT help frozen shoulder?
Evidence suggests it may reduce risk. The 2023 Duke analysis of 1,952 menopausal women found women not on HRT had nearly twice the odds of adhesive capsulitis (3.95% on HRT vs 7.65% off HRT). HRT is not a treatment for an existing frozen shoulder, but for a woman with overlapping perimenopause symptoms it is a reasonable conversation to have.
How long does frozen shoulder last in menopause?
Untreated, one to three years through freezing (2–9 months), frozen (4–12 months), and thawing (6–24 months) stages. With PT plus a steroid injection most women regain meaningful function in 6–12 months.
Should I take estrogen if I have frozen shoulder?
Frozen shoulder by itself is not a stand-alone indication for HRT, but it is a useful data point. If frozen shoulder appeared alongside hot flashes, sleep disruption, perimenopause joint pain, perimenopause hip pain, or vaginal dryness, those symptoms together — not the shoulder alone — typically guide the HRT decision. The frozen shoulder menopause overlap is exactly the kind of multi-symptom picture that benefits from a systemic conversation rather than another single-joint visit. Talk to a clinician about whether systemic estradiol is appropriate for your full picture.
What is the difference between frozen shoulder and a rotator cuff injury?
Rotator cuff problems usually have a clear injury moment, hurt with specific motions, and respond to PT. Frozen shoulder arrives with no injury, hurts deeply at night, and progressively loses range of motion in every direction. The clinical tell: in frozen shoulder, the joint is stiff even when someone else moves it for you. Rotator cuff problems do not produce that capsular stiffness.
Why is frozen shoulder more common in women?
Strong sex dimorphism — women aged 40 to 60 are several times more likely than men of the same age. The leading explanation is hormonal: estrogen stimulates collagen synthesis, reduces inflammation, and maintains connective tissue integrity. As estrogen declines, the shoulder capsule becomes more susceptible to fibroblast activation and excess collagen deposition. The same mechanism explains why menopause and joint pain travel together.
Can I prevent frozen shoulder during menopause?
No proven prevention protocol, but evidence-supported risk-reduction includes: daily shoulder mobility work, blood sugar control (diabetes is a strong independent risk factor), treating thyroid disease, staying active, and — based on the 2023 Duke data — discussing HRT if other menopause symptoms are present. The frozen shoulder menopause story is partly preventable when the underlying systemic environment is addressed early.
What kind of doctor treats menopause-related frozen shoulder?
Most women see two clinicians: an orthopaedic surgeon or sports-medicine physician for the shoulder itself, and a menopause-trained clinician for the hormonal picture. Asking the orthopaedist "is there a hormone connection here?" often surfaces the menopause angle a single-specialty visit misses.
Does frozen shoulder come back on the other side?
Yes — about 6 to 17% of women with frozen shoulder on one side develop it on the other within five years. The contralateral risk is why addressing the systemic estrogen environment matters, not just the shoulder in front of you.
Sources & references
- Saltzman E, Kennedy J, Ford A, Wittstein JR, et al. Is Hormone Replacing Therapy Associated with Reduced Risk of Adhesive Capsulitis in Menopausal Women? Orthop J Sports Med. 2023;11(7 suppl 3):2325967123S00174. PMC10392282
- Navarro-Ledesma S. Frozen Shoulder as a Systemic Immunometabolic Disorder. J Clin Med. 2025;14(20):7315. doi:10.3390/jcm14207315
- St. Angelo JM, Fabiano SE. Adhesive Capsulitis: Diagnosis and Management. AAFP. 2019. aafp.org
- Catapano M, et al. Evidence for Combining Conservative Treatments for Adhesive Capsulitis. Ochsner J. 2024;24(1):47–52. PMC10949050
- Duke Health: Hormone Therapy Reduces Risk of Shoulder Pain in Older Women. Oct 2022. corporate.dukehealth.org
- Pandey V, Madi S. Clinical Guidelines in the Management of Frozen Shoulder. Indian J Orthop. 2021. PMC8046676
- Internal: menopause statistics 2026 · symptom hub · perimenopause vs menopause
Talk to a board-certified MD about the whole picture
Frozen shoulder, sleep, periods, mood, hot flashes, joint pain — tell a clinician about all of it in one visit. ClearedRx prescribes FDA-approved or compounded HRT based on what fits, starting at $19 the first month, then $39/month ongoing, with 24-hour MD review and free shipping in all 50 states.
Find out if HRT is right for me



